(and how problems here can cause lower back, neck and shoulder issues)
By Janet Fabbri – Musculoskeletal Physiotherapist
The thoracic spine
The thoracic spine, or mid back, is made up of 167 joints! These can all be a potential source of pain or stiffness, which can cause other issues elsewhere in the body. There are 12 spinal vertebrae, which each have a disc in between them, as well as a pair of facet joints on either side, and 12 ribs join on to each thoracic vertebral joint segment, via 2 joints each. At the front the ribs join the sternum via cartilage. The thoracic spine holds up the rib cage, and many muscles need to work to hold upright posture and to allow a secure base for the limbs to be able to move optimally. This secure base can also move.
Thoracic mobility is an imperative part of human movement. If you lack mobility through the thoracic spine you will be more likely to get more injuries involving the shoulder and neck, as well as having an increased prevalence of low back pain.
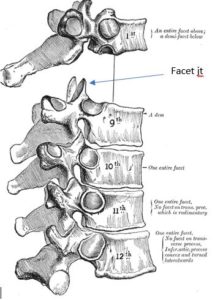
Due to the orientation of the facet joints (see blue arrow above), which join the vertebra, on average, each thoracic vertebra can rotate approximately 3 °. Therefore, the entire thoracic spine should demonstrate between 30 -35 ° of total rotation to each side (Neumann, 2010). It also moves well into side bending, or lateral flexion, which is restricted by rib compression. Alternatively, the Lumbar spine (lower back 5 vertebrae) moves a lot less into rotation and lateral flexion, but it moves mainly into forwards and backwards, due to a different orientation of these facet joints. If there is reduced movement in the thoracic spine into rotation then the lumbar spine can overly rotate, which it is not designed to do , and this can lead to disc and facet joint degeneration ( Bogduk & Twomey, 1987). If the lumbar spine is put under stress then the lower 2 joints, L4/5 and L5/S1, can become too flexible, and lose some of their stability, requiring the “core” stability muscles of the spine to have to work harder than they usually do. This disc and facet joint degeneration can lead to pain, which further inhibits the core stability muscles. The result is that the strong power muscles of the spine then goes into spasm to hold the lumbar spine, because the ligaments and deep stabilising muscles are not able to function optimally. This can be felt as the pain and stiffness you can feel in the lower back when you bend forward to put on socks. Over time this poor biomechanical pattern can lead to nerve compression and Sciatica.
How can pain in my back relate to my neck and shoulders?
The same principle applies to the neck , where if there is stiffness in the mid thoracic spine causing limited rotation and extension (arching back) then the lower neck joints ( C5/6, C6/7, C7/T1) are forced to move too much, and over time can degenerate and cause degeneration of the disc and facet joints as well as weakness of the deep core neck muscles (Jull et al 2008). This can cause a nerve root compression, and nerve pain radiating into the arm and hand.
To move the arm into full shoulder flexion (lifting the arm forward and up) requires the thoracic spine to move into extension. During shoulder flexion, the scapula upwardly rotates and posteriorly tilts on the rib cage, which encourages thoracic extension. Therefore, if the thoracic spine cannot extend, the scapula cannot posteriorly tilt, and the glenohumeral joint ( which is made up of the glenoid fossa of the scapula = the socket, and the head of the humerus =ball of the ball and socket shoulder joint) cannot get to full flexion, which increases the risk of shoulder impingement.
Your Physio can identify these issues and it can be quite complex. We can help with:
- thoracic spine mobility exercises that are specific to you, which are either flexion, extension, rotation or lateral flexion,
- target specific weaknesses in the thoracic spine, and prescribe strength
- improve core stability of the thoracic and lumbar spine as well as scapular stability.
Our Clinical exercise classes (Matwork, Reformer and other classes) also address these issues, or an individualised independent gym program using the Pilates Trapeze table, barrel, Reformer, Wunda Chair and foam roller can be used. Here are some examples:


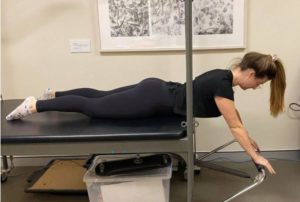

Click here to find out more about our Clinical Exercise Classes
References:
Neumann, D. A. (2010). Kinesiology of the musculoskeletal system: Foundations for rehabilitation (2nd ed.). St. Louis, MO: Mosby Elsevier.
Bogduk, N, Twomey, L.T (1987) Clinical Anatomy of the Lumbar Spine. Churchill Linvingstone.
Jull, G, Sterling, M, Falla, D, Treleavan, J, O’Leary, S ( 2008) Whiplash, Headache and Neck Pain, Churchill Livingstone.
DMA Clinical Pilates


